Aaron* underwent hernia repair and ileostomy refashioning surgery following complications from his original stoma formation. Aaron was experiencing increasing pain from incisional hernias.
Managing Complex Stoma Care Post-Surgery
*The case study presented is based on a real patient experience; identifying details have been anonymised to protect patient confidentiality.
Authors: Anna Moseley, Community Nurse Specialist.
Clinical Need: Clinical intervention for pouch leakage and peristomal skin complications with challenging skin folds and dehisced wounds.
Care Pathway: Aura® Plus Soft Convex.
Aaron underwent hernia repair and ileostomy refashioning surgery following complications from his original stoma formation. He had his stoma formed in February 2018 for colitis and had been managing it successfully. However, in 2024, he was experiencing increasing pain from incisional hernias. During his elective hernia repair, a twisted bowel was discovered that required his ileostomy to be refashioned.
Patient assessment
Aaron self-referred through the SecuriCare website and was seen one-week post-discharge. He was unable to achieve pouch adherence due to the challenging position of his stoma and the presence of an open wound. He lives with his wife and young family and had been independently managing his stoma care.
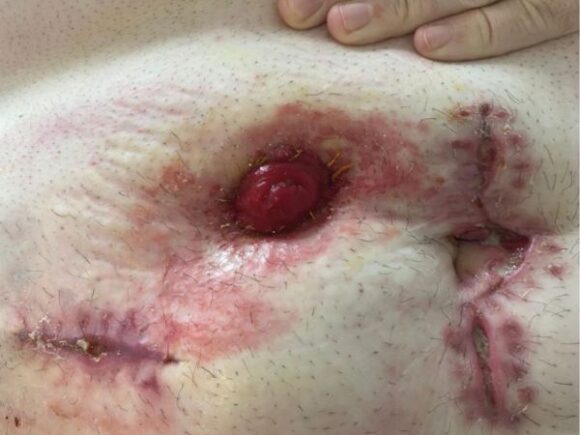
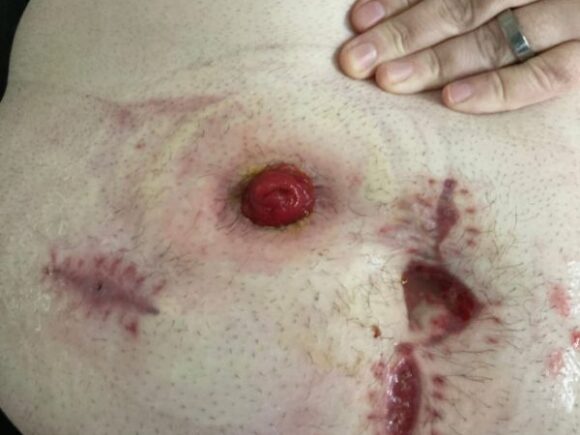
During assessment at home, Aaron mentioned he was using up to 10 pouches daily due to the pouch no longer being suitable for his needs. His stoma was positioned in a skin fold near his navel, adjacent to a dehisced abdominal wound. The stoma was producing watery output, likely exacerbated by Aaron’s poor appetite following surgery. His skin was red and irritated with signs of peristomal skin damage.
Clinical need
Aaron required immediate clinical intervention to address multiple complex issues:
- Prevention of pouch leakage through appropriate stoma support
- Management of challenging stoma positioning within skin folds
- Stoma care routine to allow for healing of nearby wounds
- Management of difficult watery stoma output
- Treatment for existing peristomal skin damage and protection to prevent further deterioration
Care pathway
The initial treatment plan included:
- Application of Aura Plus Soft Convex, chosen to provide support around the creases and skin folds around the stoma and due to the skin-friendly properties of the hydrocolloid
- Addition of a support belt to improve pouch positioning and security within the skin crease
- Application of HydroFrame with Manuka honey flange extenders to enhance pouch adherence and to protect the dehisced wound
A follow-up call was scheduled for two days later and details were provided to enable the patient to call if there were any issues, with a home visit planned for the following week.
Clinical outcome
During the follow-up call, Aaron reported significant improvement. The pouch had lasted 12 hours without leakage, allowing him to rest properly for the first time since surgery.
During the home visit follow up, peristomal skin condition showed notable improvement. Aaron was no longer changing his pouch multiple times daily, as the soft convex pouch now adhered effectively to his abdominal contours. The care plan was adjusted to daily pouch changes.
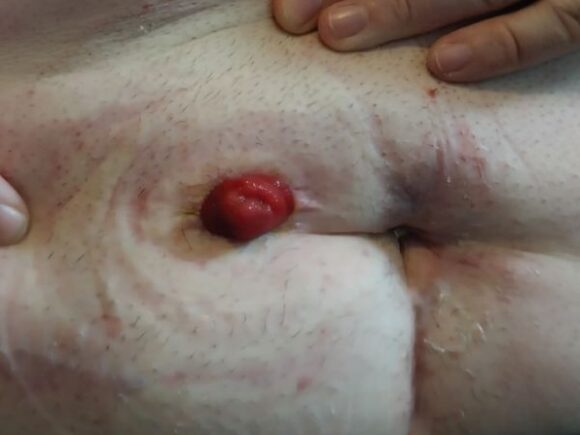
At the one-month follow-up visit, Aaron’s abdominal wound had healed completely, and his peristomal skin remained intact. He was successfully changing his pouch every 2–3 days with no further leakage issues.
Overview
Aaron described his initial situation as “dire” with frequent pouch leaks significantly impacting his post-surgical recovery and quality of life. The introduction of the Aura Plus Soft Convex pouch system, combined with appropriate accessories and support products, successfully eliminated leakage issues. This intervention not only improved his peristomal skin health but also substantially enhanced his quality of life during recovery.