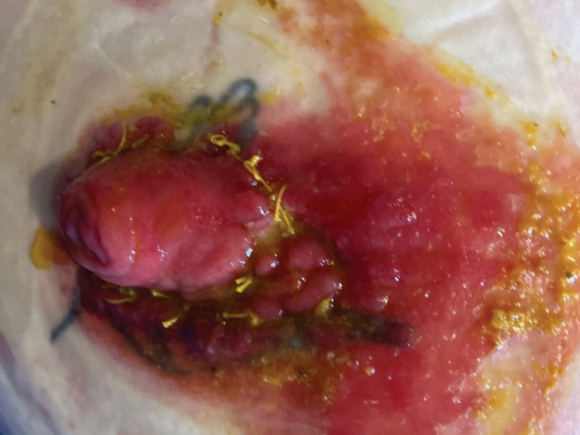
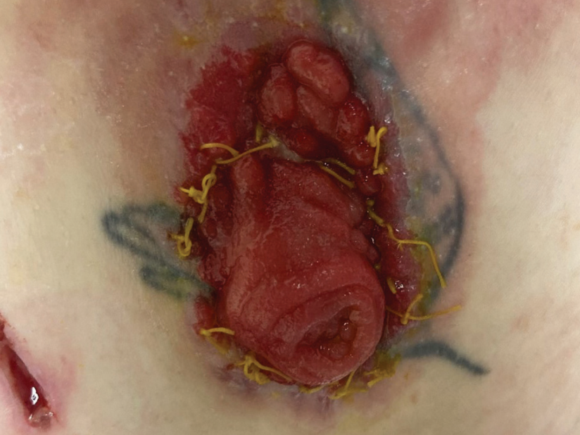
Lisa* underwent an emergency laparotomy with a small bowel resection and double-barrelled ileostomy due to a bowel perforation after an elective caesarean section. Lisa received support to manage changes in the size and shape of her stoma and abdomen, frequent leaks, peristomal skin complications, and inconsistent output.
Managing Leakage and Moisture Associated Skin Damage
*The case study presented is based on a real patient experience; identifying details have been anonymised to protect patient confidentiality.
Authors: Ruth Hetherington, Stoma Care Nurse, SecuriCare Medical.
Clinical Need: Lisa needed clinical intervention for frequent pouch leakages and resultant Moisture Associated Skin Damage (MASD).
Care Pathway: Aura® Plus Soft Convex.
This case study details how Lisa received community-based Stoma Care Nurse support to manage post-operative and postpartum challenges. These included changes in the size and shape of her stoma and abdomen, frequent leaks, peristomal skin complications, and inconsistent output. Various interventions were implemented to help Lisa adjust to life with a stoma.
Patient assessment
Lisa has a history of Crohn’s disease and an ileocecal resection. After her small bowel resection and ileostomy formation, she recovered in the Intensive Care Unit and was later transferred to a surgical ward before being discharged home.
During the initial post-discharge assessment, Lisa reported frequent pouch leakages. Her skin was red, excoriated, and weeping, causing pain and discomfort. The assessment confirmed Moisture Associated Skin Damage from prolonged exposure to stoma effluent.
Lisa was anxious due to frequent pouch leakages and painful skin, which were causing distress and affecting her self-confidence. She felt she was missing out on caring for her newborn because of the challenges with her stoma management
Clinical need
The intervention aimed to manage leakage episodes and treat damaged peristomal skin. The proximal lumen was well spouted, while the distal lumen was flush to the abdomen, passing small amounts of clear mucus. The stoma template was revised to incorporate both bowel lumens, considering potential changes in the size and shape of the stoma and abdomen.
Care pathway
To address Lisa’s skin condition and manage the frequent pouch leakages, stoma powder was incorporated into her stoma pouch change routine. This powder was added to absorb moisture and keep the skin around the stoma dry, creating an environment conducive to healing. During a detailed demonstration, Lisa was shown how to apply the stoma powder evenly around the stoma to ensure maximum absorption and protection.
Lisa was also provided with samples of Aura Plus, a product chosen for its ability to reduce the risk of leaks and promote healthy skin around the stoma. Aura Plus features an all-natural hydrocolloid containing Manuka honey. This hydrocolloid helps to reduce sensitivity and irritation while its highly absorbent formulation keeps the skin dry.
The demonstration included instructions on how to properly apply the pouch, ensuring a secure seal to prevent leaks.
Recognising the potential changes in the size and shape of Lisa’s stoma and abdomen, samples of both Aura Plus and Aura Plus Soft Convex were provided. Lisa initially chose to use Aura Plus, which has a flat flange, but she had the option to switch to Aura Plus Soft Convex if her stoma and abdomen changed and required additional support. The demonstration highlighted the differences between the flat flange and Soft Convex, explaining how the convex shape helps the stoma protrude into the pouch for better drainage
Clinical outcome
Five days after the initial intervention, Lisa had a follow-up review. During this period, she experienced no leaks and was able to use each stoma pouch for 24 hours. The assessment revealed a significant improvement in the condition of her peristomal skin, with no pain or discomfort reported. Lisa shared that she had been able to take her baby out for a walk, go shopping, and meet a friend for lunch, appearing much more positive and energetic. Another review was scheduled, with advice to continue monitoring her stoma and abdomen for any changes.
Lisa was reviewed again after fifteen days. During this period, she had spent four days in the hospital due to an abdominal collection. She received intravenous antibiotics to manage the suspected infection and continued taking oral antibiotics after being discharged. As a side effect of the antibiotics, her stoma output was liquid. Additionally, Lisa’s abdomen had reduced in size, and the proximal lumen was no longer well spouted. This combination of liquid output and changes in her abdomen meant that effluent was seeping behind the flat flange of the stoma pouch, causing further irritation.
To address these issues, Lisa was recommended to use Aura Plus Soft Convex, which would help the stoma protrude into the pouch and allow the output to drain properly, preventing it from seeping behind and irritating the peristomal skin. This intervention aimed to allow the peristomal skin to recover, as previously demonstrated with Aura Plus and stoma powder. The stoma template was revised to accommodate the changes in the size and shape of the stoma. Additionally, Loperamide was prescribed to help thicken the output.
Three days later, Lisa was reviewed again. The faecal output had thickened to a porridge-like consistency by taking Loperamide before meals.
After the infection had settled, Lisa stopped taking the antibiotics and her appetite improved. She began eating a low-residue diet to reduce the amount of undigested food. A week later, during a follow-up, Lisa confirmed that she was not experiencing any leakages and that her peristomal skin had fully improved.
Overview
This case study underscores the crucial role of the Stoma Care Nurse in supporting patients, particularly during the post-operative phase. The clinical intervention effectively managed the practical aspects of stoma care, addressing pouch leakage and improving the condition of peristomal skin affected by Moisture Associated Skin Damage (MASD). The use of Aura Plus significantly improved the skin condition around the stoma and resolved recurring leakage episodes.
Supporting a patient in the postpartum period highlighted the need for adaptability and regular monitoring. Post-surgery and post-pregnancy changes in the size and shape of the abdomen necessitated adjustments to both the stoma template and pouch. Lisa transitioned from using Aura Plus to Aura Plus Soft Convex to prevent leaks and promote healthy peristomal skin.
Initially, Lisa was anxious and distressed due to frequent leakages and painful skin, which impacted her ability to care for her newborn.
The adaptable clinical intervention, including regular monitoring, follow-ups, and the introduction of Aura Plus, significantly improved her stoma management. This allowed Lisa to focus on her new family without additional stress from stoma care.