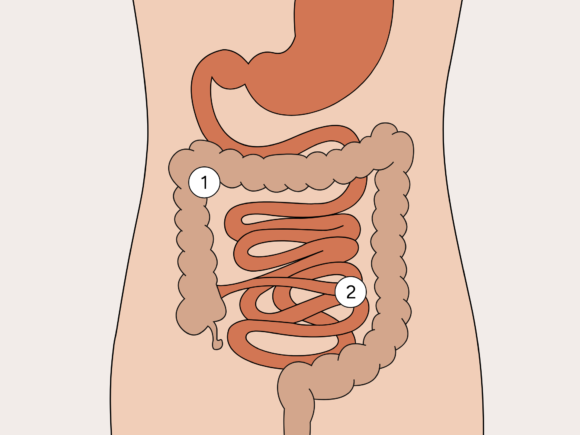
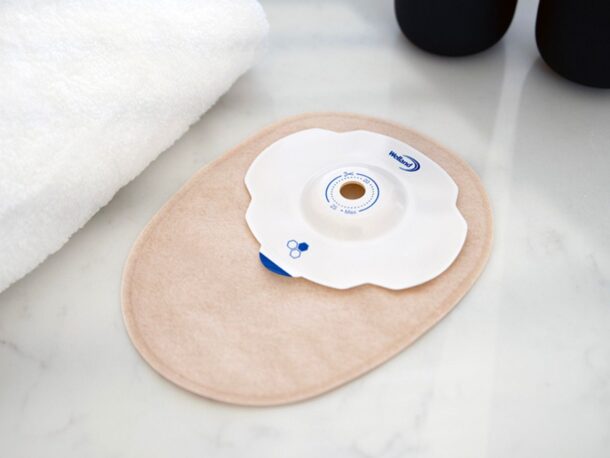
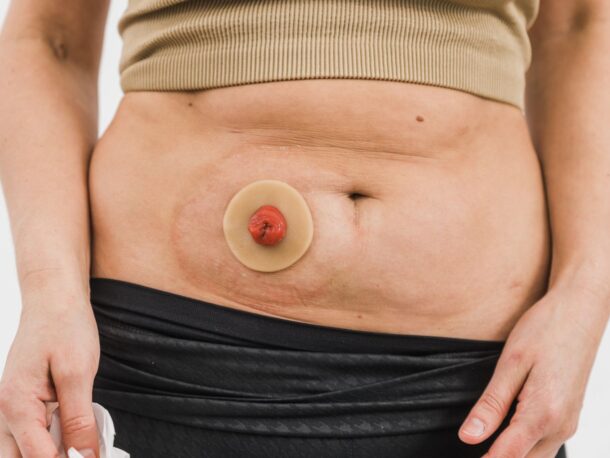
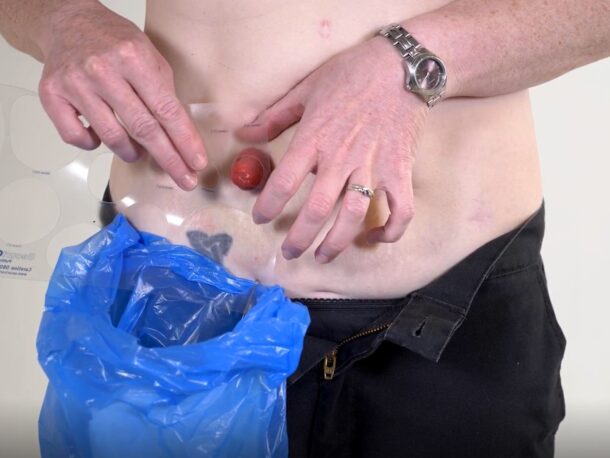
A stoma is where a part of the small intestine (labelled 2 in the diagram) or large intestine (labelled 1 in the diagram) is brought through a small opening in the surface of the abdomen to divert the flow of urine or faeces which is referred to as output. The output is collected in a bag that attaches to the abdomen. Stomas can be temporary or permanent, depending on the person’s condition and the type of surgery performed.
There are a number of conditions that may require treatment with a stoma including cancer, Crohn’s disease and ulcerative colitis. Having a stoma can represent a big improvement in a person’s quality of life and around one in 335 people living in the UK have a stoma and use stoma bags or pouches.